MRSA survivor Bill Schmelzer shares his story and the unanswered question behind his infection, and why overlooked vectors like stethoscope diaphragms demand attention.
Key Takeaways
- I developed life-threatening level 3 Sepsis from MRSA bacteremia after routine surgery despite no prior colonization
- Many healthcare-associated infections come from unknown external sources
- Research shows stethoscopes can carry MRSA and other pathogens at levels similar to clinicians’ hands
- Closing the stethoscope hygiene gap is critical to preventing infections like mine
A Routine Surgery That Wasn’t Routine
In January 2016, I underwent what was supposed to be a straightforward total hip arthroplasty.
I had reached a point where the pain in my hips was no longer manageable. Otherwise, I was healthy. My labs were normal. I had no underlying conditions that would put me at higher risk. As part of the preoperative process, I was screened for methicillin-resistant Staphylococcus aureus (MRSA). The culture was negative.
The surgery itself went as planned.
A few days later, things began to change.
There was swelling in the extremity. Then a fever. Within a short period of time, my condition deteriorated in ways that were difficult for my family to fully understand. I became confused. My speech changed. By the end of that week, I was no longer able to communicate clearly.
I was readmitted post-op day 10, the diagnosis of septic bacteremia/MRSA came on day 14.
The shift from routine recovery to a life-threatening infection happened in a matter of days.
Living With the Question
Because of my background in infection prevention, I understood what this diagnosis meant. I also understood something else that has stayed with me since.
I was not colonized with MRSA before surgery, then the infection did not originate from me.
In infection prevention terms, that distinction matters. Some infections are endogenous, meaning they come from the patient’s own flora. Others are exogenous, introduced from the environment or through contact during care.
In my case, the evidence pointed to an external source.
That leads to a difficult question.
Where did it come from?
That question has never been answered, no Root Cause Analysis was done. Even with the progress that has been made in infection prevention, there are still cases where we cannot identify the source. For patients, that uncertainty does not go away. It stays with you.
Transmission Does Not Require a Major Failure
When people think about infection risk, they often picture a breakdown in sterile technique or a missed step in a protocol.
In reality, transmission can occur in far more routine ways.
Healthcare is built on constant interaction. Patients are examined, reassessed, and monitored throughout the day. Each interaction involves contact, and each point of contact carries some level of risk.
In that environment, bacteria do not need a major lapse to move from one place to another. They only need a pathway, a vector.
Over time, I found myself returning to a simple observation.
Something was carrying bacteria.
The Clinician’s Third Hand: The Stethoscope Diaphragm Is Routinely Contaminated With MRSA and Other Resistant Pathogens
Among the many surfaces and tools used in patient care, some receive more attention than others. Hands have been the focus of decades of research and behavior change efforts, and for good reason. What about other surfaces?
One vector of concern is the “Clinician’s Third Hand”, the stethoscope diaphragm, which comes into direct contact with patients often.

Work led by Didier Pittet, the infectious disease expert who helped integrate workflow-compatible alcohol dispensers into modern care through the CDC’s 2002 hand hygiene guidelines, has shown strong evidence that the stethoscope diaphragm acts as a vector for pathogen transmission.1
He demonstrated that after a single patient exam, the diaphragm of a stethoscope can become contaminated with bacteria, including MRSA, at levels comparable to a clinician’s hands. In some cases, contamination has been detected even before patient contact, suggesting that the device itself can serve as a reservoir.
The stethoscope diaphragm was the second most contaminated surface, with MRSA among the pathogens identified, second only to clinicians’ fingertips.¹

What is more concerning is not just the contamination, but the lack of consistent systems to address it.
In many hospitals today, there is still no standardized policy or procedure ensuring stethoscope hygiene between patients.
That is not an individual failure. It is a systemic one.
Without reliable processes, even well-intentioned clinicians are left to depend on memory and time in fast-paced environments. The result is variability, and variability creates risk.
This leaves patients in a position of exposure to pathogens that can be life threatening.
The Gap Between Intention and Practice
Most clinicians are aware that stethoscopes should be cleaned between patients. The challenge is not knowledge. It is consistency.
Clinical workflows are fast-paced and complex. Priorities compete for attention. Even well-established practices can become inconsistent when they rely on perfect execution in every moment.
Unlike hand hygiene, which is reinforced through visibility and repetition, stethoscope hygiene often happens out of sight. There is no immediate cue, no clear signal to the patient, and no easy way to verify that it has been done.
Over time, this creates variability.
Infection prevention is not only about having the right protocols in place. It is about ensuring that those protocols are reliably carried out in real-world conditions.
Seeing It From the Patient’s Perspective
Before this happened, I understood infection prevention from a professional standpoint.
Afterward, I understood it as a patient.
What changed most was my understanding of the long-term impact. We talk about treating infections, managing infections, controlling infections. What we do not always talk about is the reality that, in some cases, we cannot eliminate them.
In my situation, the colonization/infection never went away. It has required multiple surgeries, long-term antibiotic therapy, and ongoing monitoring. At this point, it is something I live with.
There are limits to what current treatments can do. Antibiotics can suppress bacterial growth, but they do not always eliminate it. Over time, options become more limited.
That is a different way of thinking about healthcare-associated infections.
This is not always a short-term complication. For some patients, it becomes a permanent condition.
Moving Toward More Reliable Protection
Healthcare involves complexity, and uncertainty is part of that reality.
At the same time, there is an opportunity to reduce reliance on perfect behavior by designing processes that are easier to follow consistently.
In the case of stethoscope hygiene, that has led to interest in approaches that make cleanliness more immediate and more visible. Solutions such as The DiskCover System are built around that idea, providing a clean surface for each patient encounter without requiring a separate cleaning step.2
Affordable, rapid, and simple technology exists to protect patients from stethoscope contamination, making continued reliance on inconsistent manual cleaning increasingly difficult to justify.
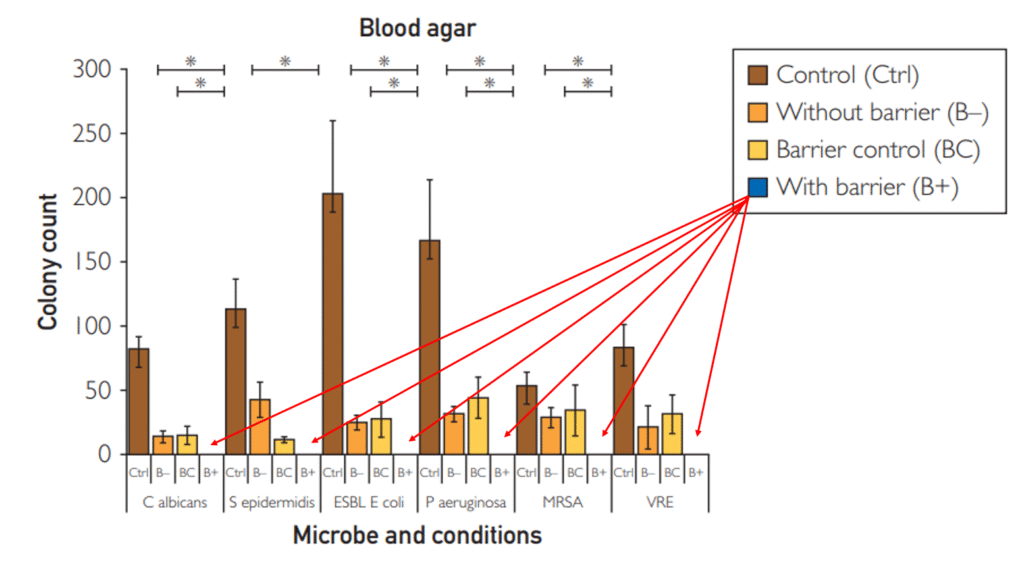
In an efficacy study, disk covers protecting contaminated stethoscope diaphragm surfaces were 100% culture negative for all tested pathogens, including MRSA
An Unanswered Question
I recovered from the sepsis event, but the question of where it came from has never been fully resolved.
That question matters, not only because of what happened to me, but because it points to something broader.
Infection prevention has made significant progress over the years. Yet there are still areas where risk is not fully addressed, often because it exists in routine, familiar parts of care.
Stethoscopes are one example.
They are used constantly. They come into direct contact with patients. And we know they can carry the same organisms we work so hard to control elsewhere.
If we are serious about reducing preventable infections, we have to be willing to look closely at those everyday moments.
That is where many of the remaining gaps still exist.
References
- Longtin Y, Schneider A, Tschopp C, et al. Contamination of stethoscopes and physicians’ hands after a physical examination. Mayo Clin Proc. 2014;89(3):291-299. doi:10.1016/j.mayocp.2013.11.016
- Vasudevan R, Shin JH, Chopyk J, et al. Aseptic Barriers Allow a Clean Contact for Contaminated Stethoscope Diaphragms. Mayo Clin Proc Innov Qual Outcomes. 2020;4(1):21-30. Published 2020 Feb 5. doi:10.1016/j.mayocpiqo.2019.10.010
Author
-
 View all posts
View all postsBill Schmelzer is an MRSA and sepsis survivor and former surgical and infection prevention professional with more than 40 years of experience in the healthcare industry. After developing a life-threatening MRSA infection following routine surgery in 2016, he gained a rare dual perspective as both clinician and patient. Today, Bill is a national speaker and patient safety advocate, sharing his story to highlight the real-world impact of healthcare-associated infections and the importance of vigilance, accountability, and infection prevention in everyday clinical practice.




