Key Takeaways
- Patients are increasingly aware of infection prevention practices during their care.
- Stethoscopes can carry contamination levels comparable to clinicians’ hands when not disinfected between patients.
- Visible hygiene practices can reassure patients and strengthen trust in the care environment.
- Emerging workflow solutions aim to ensure clean patient-contact surfaces during every examination.
Why Patients Pay Attention to Hospital Cleanliness and Infection Prevention
Patients today are more attentive than ever to the cleanliness of their healthcare environment. Research examining patient experience data has shown that perceptions of cleanliness strongly influence how patients evaluate the quality and safety of care they receive.
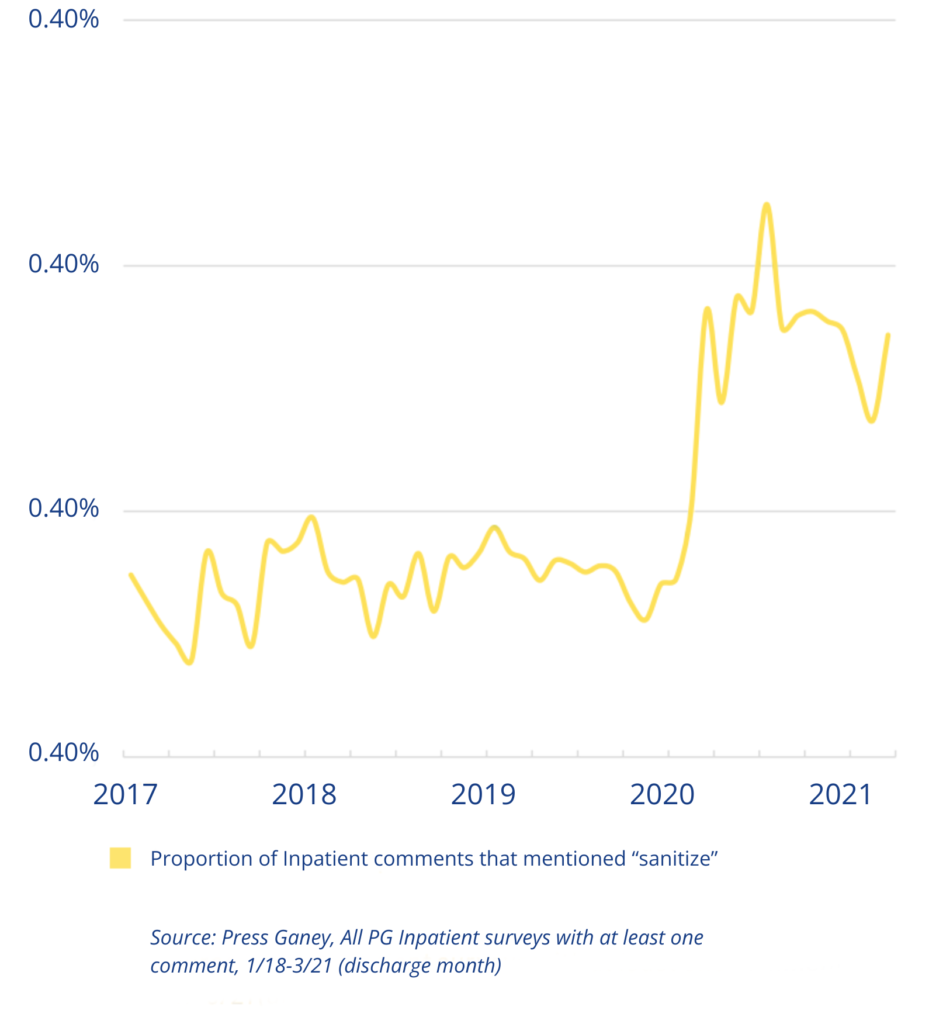
Press Ganey analysis of patient experience data has found that visible signs of hygiene, environmental cleanliness, and infection prevention practices are closely tied to patient confidence in healthcare organizations. Patients often interpret these cues as indicators of how seriously their care team takes safety and infection prevention.¹
In unfamiliar clinical environments, patients naturally look for reassurance that they are being protected from potential risks. Simple actions such as hand hygiene, the use of protective equipment, and visible cleaning practices help communicate a culture of safety.
Over the past several years, public awareness of healthcare-associated infections has also increased. Patients increasingly recognize that infection prevention involves many aspects of care, including the medical devices used during routine examinations.
One device that patients see used repeatedly throughout their care is the stethoscope.
Stethoscope Contamination and Infection Risk During Patient Examinations
Because stethoscopes are used so frequently, they also move between patients throughout the day. Research has demonstrated that stethoscope diaphragms can harbor microbial contamination similar to that found on clinicians’ hands if they are not cleaned between patient encounters.2
For patients, understanding that a device used in their examination may have contacted many other patients can raise questions about infection risk.
While clinicians are trained to follow disinfection guidelines, maintaining perfect compliance in busy clinical environments can be challenging. These realities have led infection prevention leaders to explore ways to strengthen hygiene practices around commonly used medical devices.
Cancer Patients Emphasize the Importance of Clean Stethoscopes
While patients often notice visible hygiene practices such as hand hygiene and environmental cleaning, research suggests that expectations extend to the medical devices used during examinations.
A study conducted at the Cleveland Clinic surveyed both patients and healthcare professionals regarding their perceptions of stethoscope hygiene and the use of stethoscope barriers.3 The patient cohort included immunocompromised patients receiving cancer care, where infection prevention practices are particularly critical.
During the study, patients reported that they observed irregular hygiene practices involving stethoscopes used during their care, raising concerns about whether the device had been cleaned between patient encounters.
When asked to rate the importance of a stethoscope being clean before it touches them, patients gave the practice the highest possible importance rating, averaging 100 out of 100 on a 100-point scale.
For many patients, the stethoscope is one of the most visible medical tools used during examinations. Seeing the same device used repeatedly across multiple patient encounters can lead patients to question whether the contact surface has been disinfected.
These findings reinforce a broader trend seen in patient experience research: visible infection prevention practices help patients feel safer and more confident in their care environment. Ensuring that examination devices begin each patient encounter with a clean contact surface may therefore support both patient safety and patient trust.
How Visible Infection Prevention Practices Improve Patient Confidence
Patients often interpret visible safety practices as a reflection of the overall quality of care they are receiving.
When infection prevention steps are clearly observable, they can help reassure patients that their care team is actively protecting them from potential risks. For example, watching a clinician perform hand hygiene before an examination signals a commitment to patient safety.
The same principle applies to the tools used during care.
If patients see that a clean patient-contact surface is being used during their examination, it reinforces the perception that infection prevention is being taken seriously. These visible safeguards can be especially meaningful for individuals who are already anxious about their health or hospitalization.
In this way, infection prevention practices can contribute not only to patient safety but also to patient confidence.
Why Stethoscope Hygiene Compliance Can Be Challenging in Clinical Workflows
Guidelines recommend disinfecting stethoscopes between patient encounters. However, studies have shown that achieving consistent compliance with these recommendations can be difficult in real-world clinical settings.
Healthcare providers often work in fast-paced environments where examinations must occur quickly and efficiently. Ensuring that every stethoscope surface is disinfected thoroughly between patients can be challenging when clinicians are managing multiple responsibilities.
Because the stethoscope functions almost like a “third hand” during patient care, infection prevention teams have begun examining whether new approaches might better support consistent hygiene practices.
Emerging Workflow Solutions to Improve Stethoscope Hygiene and Patient Safety
To address these challenges, some healthcare organizations have explored workflow-based approaches that help ensure a clean patient-contact surface for every examination.
One example includes the use of aseptic stethoscope barriers that create a fresh contact surface for the stethoscope diaphragm before each patient encounter. Systems such as The DiskCover System automate the application of these touch-free, aseptic single-use barriers, allowing clinicians to maintain consistent hygiene without adding additional manual cleaning steps.

Because the barrier is visibly applied before the examination, patients can also see that a clean surface is being used during their care. For some healthcare organizations, this combination of safety and visibility has been an important component of improving the patient experience.
Strengthening Patient Trust Through Infection Prevention
Patient trust is built through consistent actions that demonstrate a commitment to safety.
Infection prevention practices such as hand hygiene, environmental cleaning, and device hygiene all contribute to creating a care environment where patients feel protected. While many of these precautions occur behind the scenes, visible safety measures can play a powerful role in reinforcing confidence in the care team.
As healthcare organizations continue working to reduce healthcare-associated infections, attention to commonly used examination devices such as the stethoscope may represent an additional opportunity to improve both patient safety and patient experience.
Ensuring that every patient examination begins with a clean contact surface helps reinforce a culture where safety, trust, and compassionate care remain central to the healthcare experience.
References
- Press Ganey. Emerging Best Practices in Response to Evolving Patient Perceptions of Clean. Compass One Healthcare. 2022.
- Longtin Y, Schneider A, Tschopp C, Renzi G, Gayet-Ageron A, Schrenzel J, et al. Contamination of stethoscopes and physicians’ hands after a physical examination. Mayo Clin Proc. 2014;89(3):291-299.
- Siegmund, L.A., Peacock IV, W.F., Bena, J., Morrison, S. “Patients and Healthcare Professionals’ Perceptions of Stethoscope Barriers” OJIN: The Online Journal of Issues in Nursing Vol. 29, No. 3. 2024 Sep 17.
Author
-
 View all posts
View all postsW. Frank Peacock MD, FACEP, FACC, FESC is Professor of Emergency Medicine at Baylor College of Medicine. He has authored more than 900 peer-reviewed publications on cardiovascular emergency care and infection prevention. Dr. Peacock also serves as Chief Medical Officer of AseptiScope, where he supports research and clinical education focused on stethoscope hygiene and reducing pathogen transmission in healthcare.




